Mental Health
Being mentally healthy during childhood means reaching developmental and emotional milestones and learning healthy social skills and how to cope when there are problems. Mentally healthy children have a positive quality of life and can function well at home, in school, and in their communities.
Mental disorders among children are described as serious changes in the way children typically learn, behave, or handle their emotions, which cause distress and problems getting through the day. Many children occasionally experience fears and worries or display disruptive behaviors. If symptoms are serious and persistent and interfere with school, home, or play activities, the child may be diagnosed with a mental disorder.
Mental health is not simply the absence of a mental disorder. Children who don’t have a mental disorder might differ in how well they are doing, and children who have the same diagnosed mental disorder might differ in their strengths and weaknesses in how they are developing and coping, and in their quality of life. Mental health as a continuum and the identification of specific mental disorders are both ways to understand how well children are doing.
Among the more common mental disorders that can be diagnosed in childhood are attention-deficit/hyperactivity disorder (ADHD), anxiety (fears or worries), and behavior disorders. Other childhood disorders and concerns that affect how children learn, behave, or handle their emotions can include learning and developmental disabilities, autism, and risk factors like substance use and self-harm.
Symptoms of mental disorders change over time as a child grows, and may include difficulties with how a child plays, learns, speaks, and acts, or how the child handles their emotions. Symptoms often start in early childhood, although some disorders may develop during the teenage years. The diagnosis is often made in the school years and sometimes earlier; however, some children with a mental disorder may not be recognized or diagnosed as having one.
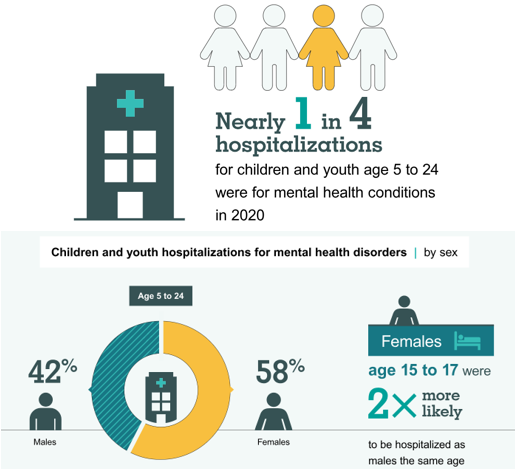
Impact of Covid-19 Pandemic on Children’s Mental Health
The COVID-19 pandemic has had a devastating impact on many children’s mental health and wellbeing. Across Canada, children’s hospitals, community hospitals, children’s rehabilitation centres, home care, palliative care and respite provider agencies report a measurable increase in concerns, visits and admissions related to mental health since the pandemic began. The prevalence of depression and anxiety symptoms amongst children during COVID-19 has doubled compared to pre-pandemic estimates. The pandemic had evoked symptoms of depression, anxiety, irritability, reduced attention span, hyperactivity, or obsessions. Children’s healthcare providers are also seeing up to a threefold increase in visits and admissions for acute and increasingly complex eating disorders.
Behaviour Disorders
The most common disruptive behaviour disorders include oppositional defiant disorder (ODD) and conduct disorder (CD). These behavioural disorders share some common symptoms, so diagnosis can be difficult and time consuming. A child or adolescent may have two disorders at the same time. Other exacerbating factors can include emotional problems, mood disorders, family difficulties and substance abuse.
Oppositional Defiant Disorder
Around one in 10 children under the age of 12 years are thought to have oppositional defiant disorder (ODD), with boys outnumbering girls by two to one.
Some of the typical behaviours of a child with ODD include:
– Easily angered, annoyed or irritated.
– Frequent temper tantrums.
– Argues frequently with adults, particularly the most familiar adults in their lives, such as parents.
– Refuses to obey rules.
– Seems to deliberately try to annoy or aggravate others.
– Low self-esteem.
– Low frustration threshold.
– Seeks to blame others for any misfortunes or misdeeds.
Conduct Disorder
Children with conduct disorder (CD) are often judged as ‘bad kids’ because of their delinquent behaviour and refusal to accept rules. Around 5 per cent of 10-year-olds are thought to have CD, with boys outnumbering girls by 4 to one. Around one-third of children with CD also have attention deficit hyperactivity disorder (ADHD).
Some of the typical behaviours of a child with CD may include:
– Frequent refusal to obey parents or other authority figures.
– Repeated truancy.
– Tendency to use drugs, including cigarettes and alcohol, at a very early age.
– Lack of empathy for others.
– Being aggressive to animals and other people or showing sadistic behaviours including bullying and physical or sexual abuse.
– Keenness to start physical fights.
– Using weapons in physical fights.
– Frequent lying.
How to Support Children with Depression
If you think your child is depressed:
Talk with your child about sadness and depression.
Kids might not know why they are so sad and why things seem so hard. Let them know you see that they’re going through a hard time and that you’re there to help. Listen, comfort, offer your support, and show love.
Set up a visit with your child’s doctor.
Let your child’s doctor know if sad or bad moods seem to go on for a few weeks. By itself, this doesn’t always mean a child is depressed. Tell your child’s doctor if you have also noticed changes in your child’s sleep, eating, energy, or effort. Tell them if your child is dealing with a loss, a big stress, or hardship. The doctor will do a physical exam. A full exam lets the doctor check for health issues that could cause your child’s symptoms. They can also check for depression. Your child’s doctor may refer you to a child therapist. The doctor’s office might have a child therapist on staff.
Set up a visit with a child therapist.
A child therapist (mental health doctor) will spend time talking with you and your child. They will do an in-depth check for depression by asking questions and listening. The therapist can explain how therapy can help your child.
Take your child to therapy visits.
The therapist may suggest a few visits, or more. Therapy can take time, but you will see progress along the way.
Be patient and kind.
When your child acts moody or difficult, try to stay patient. Talk with your child’s therapist about the best ways to respond when your child acts this way. Often, it helps to connect with your child in a calm way, then guide them to better behavior. Instead of feeling bad, this lets kids feel proud of doing better. It lets them see that you’re proud of them, too.
Enjoy time together.
Spend time with your child doing things you both can enjoy. Go for a walk, play a game, cook, read stories, make a craft, watch a funny movie. Spend time outdoors if you can. These things gently encourage positive moods. They help you and your child feel close.
How to Support Children with Anxiety
Parents and caregivers can play a big role in helping children manage their anxiety. Here are some examples:
– Help your child recognize, acknowledge, and name their feelings, including how they feel physically.
– Avoid avoidance. For strong emotions and sensitive topics, try “You look worried. Is something on your mind?”, or “It sounds like you’re really
angry. Would you like to talk about that?”
– Empathize and validate anxieties but try not to reinforce them. Try “I know you’re feeling scared, AND I know you’re brave to do this”.
– Connect and maintain secure attachment. Participate in child-led, free play with younger children, and stay aware of, and involved with
teens:
* Spend one-on-one time together.
* Know and show interest in who their friends are.
* Encourage extra-curricular activities.
– Foster self-confidence through effective praise:
* Say “You…” instead of “I…”
* Be specific about how they have earned your attention.
* Recognize brave, helpful, or kind acts as soon as possible after they happen. For younger children, notice brave behaviors, no
matter how small.
– Encourage opinions and choices. Accept growing independence in older children and promote and celebrate good decision-making and
problem-solving.
– Break the task of facing anxiety into small, practical steps, and positively reinforce each one.
– Reward attempts, and compliment process as much as end results. Focus on strengths rather than weaknesses.
– Model coping skills and techniques such as deep breathing, muscle tension relaxation, mindfulness, distraction, and positive self-talk.
– Prevent avoidance by using gentle but firm encouragement.
– Be involved with schooling. If your child or teen has anxiety, help teachers understand its sources and related behaviors. For example,
explain that when your child avoids classroom tasks or appears oppositional, this is likely due to anxiety. Make sure that necessary supports
or accommodations are in place.
– For young children showing signs of childcare or school avoidance:
* Prepare the night before so mornings are not rushed and stressful.
* Encourage bringing a favorite toy from home to ease transition.
* Take time for a warm goodbye but avoid repeated goodbyes.
– In heated family moments, take time to:
* Calm down before speaking.
* Speak slowly and clearly rather than loudly.
* Be respectful of beliefs and feelings.
* Be assertive rather than aggressive.
How to Support Children with ADHD
Parenting is as important as any other part of ADHD treatment. The way parents respond can make ADHD better or worse. If your child has been diagnosed with ADHD:
Be involved.
Learn all you can about ADHD. Follow the treatment your child’s health care provider recommends. Go to all recommended therapy visits. If your child takes ADHD medicines, give them at the recommended time. Don’t change the dose without checking with your doctor. Keep your child’s medicines in a safe place where others can’t get to them.
Know how ADHD affects your child.
Every child is different. Identify the problems your child has because of ADHD. Some kids need to get better at paying attention and listening. Others need to get better at slowing down. Ask your child’s therapist for tips and ways you can help your child practice and improve.
Focus on teaching your child one thing at a time.
Don’t try to work on everything at once. Start small. Pick one thing to focus on. Praise your child’s effort.
Work with your child’s school.
Meet often with teachers to find out how your child is doing. Work with the teacher to help your child do well.
Connect with others for support and awareness.
Join a support organization for ADHD like CHADD (Children and Adults with Attention Deficit/Hyperactivity Disorder) to get updates on treatment and info, etc.
Find out if you have ADHD.
ADHD often runs in families. Parents (or other relatives) of kids with ADHD might not know they have it too. When parents with ADHD get diagnosed and treated, it helps them be at their best as parents.
Discipline with purpose and warmth.
Learn what discipline approaches are best for a child with ADHD and which can make ADHD worse. Get coaching from your child’s therapist on ways to respond to your child’s behaviors. Kids with ADHD might be sensitive to criticism. Correcting their behavior is best done in a way that’s encouraging and supportive rather than punishing.
Set clear expectations.
Before you go somewhere, talk with your child to explain how you want them to behave. Focus more energy on teaching your child what to do, rather than reacting to what not to do.
Talk about it.
Don’t shy away from talking with your child about ADHD. Help kids understand that having ADHD is not their fault, and that they can learn ways to improve the problems it causes.
Spend special time together every day.
Make time to talk and enjoy relaxing, fun activities with your child, even if it’s just for a few minutes. Give your child your full attention. Compliment positive behaviors. Don’t over-praise but do comment when your child does something good.
Your relationship with your child matters most.
Kids with ADHD often feel they’re letting others down, doing things wrong, or not being “good.” Protect your child’s self-esteem by being patient, understanding, and accepting. Let your child know you believe in them and see all the good things about them. Build resilience by keeping your relationship with your child positive and loving.
How to Support Teens with Eating Disorders
You know your teen better than anyone. If you notice unusual behaviours and are concerned your teen may have an eating disorder, your first step will be to talk to them. Encourage them to express their worries and concerns. Use “I” statements and let them know that you are aware they are struggling. For example, you may say: “I’ve noticed that you may be going through a rough time lately. I’m happy to listen or talk and see if I can help.”
Stay calm and avoid judging or blaming your teen. A teen who is struggling with an eating disorder may resist disclosing his or her behaviours or feelings. Let your teen know you care about them no matter what and you will support them through difficult times.
Eating disorders can be prevented if action is taken at the first signs of recurrent preoccupation with body weight and image.
Teens can learn healthy ways to cope with their worries and life challenges. Parents, schools and the community all have a role to play in building healthy coping skills that will help avoid eating disorders.
If the symptoms of an eating disorder are severe, medical treatment may be needed to reverse a physical condition that could otherwise become critical. If you notice that your teen’s mental and physical health is rapidly deteriorating, don’t hesitate to seek immediate help from your primary health care provider or community health care centre.
The majority of teens with eating disorders are able to recover with support from their family, friends and community. There are many resources available across Canada that can help you find reliable information and connect to your local resources.
How to Support Children with Behavioral Disorders
The best way to support your child with behavioral disorders is treatment. Untreated children with behavioural disorders may grow up to be dysfunctional adults. Generally, the earlier the intervention, the better the outcome is likely to be.
Treatment is usually multifaceted and depends on the particular disorder and factors contributing to it, but may include:
– Parental education-for example, teaching parents how to communicate with and manage their children.
– Family therapy-the entire family is helped to improve communication and problem-solving skills.
– Cognitive behavioural therapy-to help the child to control their thoughts and behaviour.
– Social training-the child is taught important social skills, such as how to have a conversation or play cooperatively with others.
– Anger management-the child is taught how to recognize the signs of their growing frustration and given a range of coping skills designed to
defuse their anger and aggressive behaviour. Relaxation techniques and stress management skills are also taught.
– Support for associated problems-for example, a child with a learning difficulty will benefit from professional support.
– Encouragement-many children with behavioural disorders experience repeated failures at school and in their interactions with others.
Encouraging the child to excel in their particular talents (such as sport) can help to build self-esteem.
– Medication-to help control impulsive behaviours.
Parent Programs
These programs can help you:
– Respond in a positive way when your child asks for help or wants attention.
– Choose realistic goals for your child.
– Better monitor your child’s behavior.
– Learn more effective parenting skills.
– Have more confidence in being able to handle situations.
– Reduce your stress.
The programs help support you and can teach you specific ways to help change your child’s behavior without shouting, threatening, or using physical punishment. You can learn to:
– Set clear rules.
– Stay calm when asking your child to do something.
– Make sure your instructions are clear and right for your child’s age.
– Explain the consequences of disruptive behavior to your child.
– Respond to disruptive behavior with things such as quiet time or a time-out.
You can also learn ways to help support your child and:
– Improve your child’s social skills.
– Help your child build friendships.
– Help your child learn how to control his or her emotions.
– Teach your child problem-solving skills.
– Help your child learn to be independent.
Child Programs
These programs can help children:
– Feel more positive about themselves and their family.
– Strengthen their social, communication, and problem-solving skills.
– Better communicate feelings and manage anger.
– Practice good behaviors.
Teen Programs
For teens, a trained therapist may meet with parents and also with the whole family together. The therapist may look for patterns in the way family members interact that could cause tension and problems. The therapist can then help your family learn new ways to communicate to avoid conflict.
The therapist can help you learn how to:
– Be more involved with your teen.
– Set clear rules and consequences for breaking the rules.
– Improve your leadership, communication, and problem- solving skills.
– Support your teen.
Resources
Kid Help Phone
You can reach a professional counsellor at Kids Help Phone in English or French 24/7 by calling 1-800-668-6868. Our phone service is also offered in over 100 languages including Plains Cree, Severn, Ojibwe, Ukrainian, Russian, Pashto, Dari, Mandarin and Arabic with the help of trained interpreters.
Talk Suicide Canada
If your child talks about suicide, self-harm, a mental health crisis, a substance use crisis, or any other kind of emotional distress, get help right away. Call Talk Suicide:
Canada: 1-833-456-4566 or text 45645 (4 p.m. to midnight ET).
Youth Mental Health Services in BC Map
https://helpstartshere.gov.bc.ca/
Anxiety Resources for Kids
https://maps.anxietycanada.com/courses/anxiety-plan-children-teens/
CHADD (Children and Adults with Attention Deficit/Hyperactive Disorder)
https://chadd.org/
Eating Disorder Association of Canada
https://edac-atac.com/
Richmond Early Childhood Mental Health Program
https://vch.eduhealth.ca/en/viewer?file=%2fmedia%2fVCH%2fGK%2fGK.700.R53.pdf#search=mental%20health%20children&phrase=false
Alan Cashmore Centre
https://vch.eduhealth.ca/en/viewer?file=%2fmedia%2fVCH%2fGK%2fGK.700.A43.pdf#search=mental%20health%20children&phrase=false
